Diabetes is a disease that impacts your entire life. Because it deals with blood sugar, every part of the body that receives blood flow is affected. This is common knowledge for most people, but despite that, many of us fail to consider the impact diabetes can have on our eyes when we think about the potential complications of diabetes. People with diabetes are at an increased risk of vision loss due to a wide range of diseases and conditions.
It is absolutely crucial that we understand the impact diabetes can have on our eyes. Today, we are going to discuss diabetes and how it interacts with our eye health.
What is Diabetes?
Before we consider the eye health impact of diabetes, we should spend some time discussing the disease in general. Most people are familiar with the term diabetes and have a general idea of what it entails, but they may not know the specifics.
Generally speaking, diabetes is a condition that impacts the production and absorption of insulin: the hormone that regulates the amount of sugar in your blood.

There are two main types of diabetes which interact differently with your body.
Type 1
Type 1 diabetes is a kind of autoimmune disorder. When your natural immune system starts to injure cells in your pancreas, your body can no longer produce insulin properly.
This type of diabetes is usually genetic. However, it can occur as a result of certain infections or viruses.
Type 2
Type 2 diabetes occurs when the body becomes resistant to the effects of insulin. As a result, blood sugar levels become harder to regulate. Eventually, the body may stop producing insulin altogether.
This type of diabetes often occurs as the result of lifestyle factors, including:
- Sedentary living
- Obesity
- Diet
- Smoking
- High cholesterol
There are also natural risk factors, such as age and ethnicity.
How Can Diabetes Affect My Vision?
Diabetes is not necessarily a guarantee of other eye health issues. However, it can certainly increase your risk of conditions like glaucoma, cataracts, and age-related macular degeneration.
Glaucoma
Glaucoma is a condition that causes progressive damage to the optic nerve, which is responsible for sending signals from your eyes to your brain. Glaucoma is often associated with an increase in intraocular pressure, however, that is not always the case.
Diabetes increases your risk for a specific type of glaucoma called neovascular glaucoma. When blood vessels become damaged, the body may try to replace them by growing new ones.
These new blood vessels can be irregular, growing on the iris. As new blood vessels grow on the iris, they disrupt the flow of intraocular fluid called aqueous humour. This disruption causes intraocular pressure to rise, which damages the optic nerve.
Cataracts
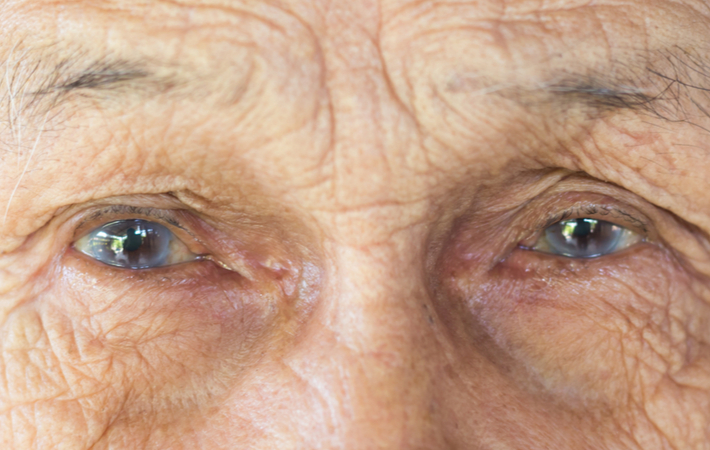
Cataracts occur when the proteins in your eye’s crystalline lens start to restructure, leaving less space for light to pass between them. As a result, your vision can become cloudy with more muted colours.
Diabetes can increase your risk for cataracts because unregulated blood sugar causes the lens to swell. As it swells, the proteins may restructure faster than they would naturally, leading to earlier cataract development.
AMD
The macula is a small portion of the retina, which is responsible for detail vision, allowing us to recognize numbers, read words, notice faces, and more.
Age-related macular degeneration or AMD is a condition that occurs when the macula sustains permanent damage. The most severe kind of AMD is called wet macular degeneration. This occurs when your body tries to replace damaged blood vessels by growing new ones. However, the new blood vessels are often weak and irregular, and can lead to bleeding and the development of scar tissue.
Diabetes increases your risk of AMD because high blood sugar levels can damage your retinal blood vessels more quickly. The more damaged blood vessels you have, the more likely your body is to replace them with weak and irregular blood vessels.
Diabetic Eye Disease
There’s one condition that is unique to people with diabetes, which we call diabetic eye disease. This condition occurs in two forms: diabetic retinopathy and diabetic macular edema.
Diabetic Retinopathy
Diabetic retinopathy occurs when the blood vessels in the retina sustain damage from high blood sugar levels. Your body tries to replace the damaged blood vessels by growing new ones. However, the new blood vessels are weak and irregular. They often result in leakage and the development of scar tissue. This scar tissue makes it more difficult for your retina to perceive light.
Diabetic Macular Edema
If diabetic retinopathy is left untreated, it can develop into diabetic macular edema. As the irregular blood vessels continue to leak into the retina, the layers of retinal tissue start to swell. Eventually, they swell so much that they obscure or overtake the macula. This damages macular cells and can cause permanent loss of central vision.
Patients With Diabetes Need Frequent Eye Exams

If you have diabetes, it is absolutely crucial that you receive an eye exam at least once a year, or as often as recommended by your optometrist. Although you may not notice any changes to your vision, it’s important to recognize that your eyes are always at risk. Without the appropriate insulin levels to regulate your blood sugar, your eyes will sustain damage. That damage may be slow, but it is cumulative and can result in serious consequences, including total vision loss.
However, with regular specialized eye exams, your eye doctor can track changes to your vision, detect damage before you notice any vision loss, and prescribe the appropriate treatment to preserve as much of your vision as possible.


