Glaucoma is one of Canada’s leading causes of vision loss. Approximately 400, 000 Canadians live with glaucoma, yet most of us know very little about the disease.
As an optometrist, I feel that it is very important that my patients understand any and all threats to their vision. In my opinion, glaucoma is one of the greatest threats we encounter today.
What is Glaucoma?
Glaucoma is an eye disease that causes gradual damage to the optic nerve. In many cases, the damage the optic nerve sustains is attributed to an increase in intraocular pressure. However, this isn’t necessarily the case for every type of glaucoma. Regardless, the damage glaucoma causes is permanent and irreversible.
What is Intraocular Pressure?
There is a space between your cornea and your crystalline lens called the anterior chamber. That chamber is filled with a fluid called the aqueous humour, which continuously flows into the chamber from an opening between the iris and the lens, and drains out through a drainage system at the base of the eye.
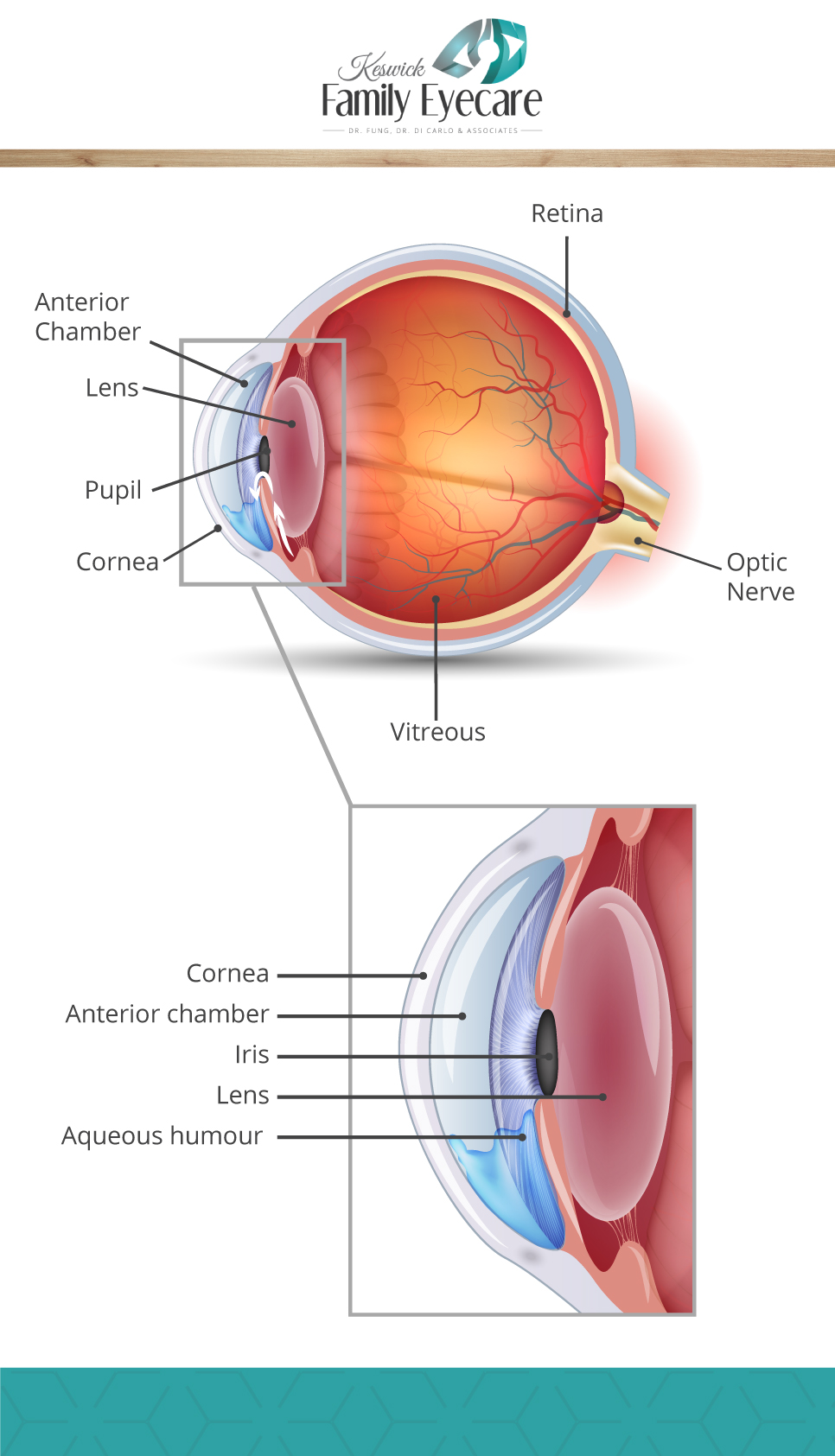
Your intraocular pressure is a metric to indicate how much aqueous humour is filling your anterior chamber.
High IOP Causes Optic Nerve Damage
The optic nerve sits at the very back of the eye. It is responsible for receiving impulses from the retina and transmitting them to your brain, which then interprets the impulses as images.
If intraocular pressure is too high, the interior part of the eye, called the vitreous, can start to press on the optic nerve, causing damage. Your optic nerve is a crucial part of the visual system. Without it, information has no way of travelling from your eyes to your brain.
Symptoms of Glaucoma
Glaucoma is sometimes called the silent thief of sight for the way it slowly destroys vision without causing many noticeable symptoms. Most patients do eventually notice some vision loss, however, by that point, they have typically undergone significant damage.
There is one type of glaucoma that does cause quite severe symptoms, which we’ll get into in just a moment.
Types of Glaucoma
Open-Angle Glaucoma
Open-angle glaucoma is the most common type of glaucoma. It occurs when there is enough space between the iris and the lens for the aqueous humour to flow into the anterior chamber, but one of the drainage ducts is blocked, causing IOP to build.
Acute Angle-Closure Glaucoma
Acute angle-closure glaucoma occurs when the opening between the iris and the lens is no longer wide enough to allow the aqueous humour to flow through. This usually happens very suddenly and causes severe symptoms. Symptoms of acute angle-closure glaucoma can include:
- Nausea
- Vomiting
- Headache
- Severe eye pain
- Excessive tears
- Blurry vision
- Glare or halos around lights
Angle-closure glaucoma is a medical emergency. If you experience these symptoms, you need to get help right away.
Normal Tension Glaucoma
In some cases, the optic nerve sustains damage without any change in intraocular pressure. The drainage ducts are fully functioning and the space between the iris and the lens is wide enough to allow the flow of the aqueous humour, but the optic nerve still suffers damage.
Doctors are still unsure why this occurs and what causes the damage.
Detecting Glaucoma
There are a number of tests optometrists use to detect glaucoma in its early stages. The one most patients are familiar with is called non-contact tonometry, which often involves trying not to blink while a machine blows a puff of air into your eye. While tonometry is a reasonably effective diagnostic tool, that test only measures intraocular pressure. As we now know, glaucoma doesn’t necessarily impact your IOP.
Luckily, in recent years, scientists have developed far more advanced methods of detecting glaucoma, sometimes earlier than we have ever been able to detect it before. At Keswick Family Eyecare, we use an OCT with some advanced functionalities to get the earliest diagnosis possible.
OCT
OCT stands for ocular coherence tomography. It is a special type of imaging equipment that allows eye doctors to see detailed images of some of the structures at the back of your eye, like the retina and the optic nerve.
Your optic nerve is made of very small fibres. These fibres are visible with an OCT, which means the doctor can evaluate the health of your optic nerve and track any changes that may occur from year to year. If your optometrist sees that the fibres of the optic nerve are sustaining damage, it can indicate the presence of glaucoma before you notice any significant vision loss.
The OCT machine we use at Keswick also offers the added benefit of colour fundus photography. A fundus camera takes real photos of your eyes’ internal structures, allowing us to see each part in more detail.
Some OCT machines also offer something called a Hood report, which compiles various data from your OCT into one comprehensive document. This makes it much easier for your optometrist to notice any changes to your eyes’ internal structures, identify the presence of glaucoma, and choose the best course of treatment early on.
Can Glaucoma Be Prevented?
As of today, we do not know of any way to prevent the development of glaucoma. However, with regular eye exams, advanced testing, early diagnosis, and the right treatments, we can manage glaucoma and prevent significant vision loss.
The most important thing to remember is that, although we can detect glaucoma earlier and earlier, you cannot detect it yourself. If you want to avoid losing portions of your vision to glaucoma, you need to see your optometrist regularly. Optometrists are here to keep your eyes healthy and your vision strong for years to come.


